“Obviously [with] any easing of restrictions, we would expect these trajectories to steepen or stay the same. We’re certainly not going to get flatter,†Mr Wallace said.
Victoria has, on average, about 400 staffed and available intensive-care hospital beds each day. The government says it can open up 1500 intensive and critical-care spaces in the public health system, which can be scaled up to 4000 spaces if faced with a coronavirus disaster far greater than the state’s second wave.
Premier Daniel Andrews admits it will be a significant challenge to staff the beds he has promised.Credit:Chris Hopkins
But reaching that 4000-bed figure could take months and if more than 1500 beds were required, staffing them could prove complicated.
The issue is politically contentious because Mr Andrews promised “an extra 4000 ICU beds†in April last year as part of a widely touted $1.3 billion package to “respond to the coronavirus pandemic and protect Victorian livesâ€.
Loading
When asked on Wednesday if there were enough nurses and other professionals to support those beds should there be a rush of gravely ill COVID-19 patients, the Premier admitted: “It will not be easy. It will be very challenging.â€
Australian Medical Association Victorian branch president Roderick McRae said he believed the 4000-beds figure was “pie in the skyâ€, and would only be possible if every worker in the hospital system was diverted to care for COVID-19 patients, and they would be unable to look after anyone else.
“The patient can’t intubate themselves,†he said.
To ensure the system is not overwhelmed, COVID-19 patients are being “streamed†into a number of designated Melbourne hospitals, including the Royal Melbourne Hospital, Monash Medical Centre, the Northern Hospital and The Alfred.
Different models of care are also being examined, such as having one critical-care nurse leading teams of two or three nurses without critical-care training, or bringing back trained nurses who had moved into research, administration or other areas.
About 1600 COVID-19 patients were also being cared for in their homes as part of a “hospital in the home†program, freeing up beds for the most serious cases. And new furloughing policies had been put in place to prevent hospitals being paralysed by staff absences during an outbreak.
Australian and New Zealand Intensive Care Society president Anthony Holle said the number of ICU beds could be expanded by moving new beds into unused areas of the hospitals. But the major limitation remained specialist staffing.
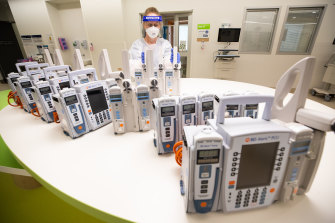
More ICU beds will need more specialist staff.Credit:Jason South
Intensive-care specialist Stephen Warrillow said work in his hospital – the Austin – had begun to make additional spaces for coronavirus patients needing intensive care. Space for 12 additional beds was being set up in part of the hospital previously used for small procedures, minor surgery and endoscopy, he said.
Much of it is similar to work done in early 2020 in Victoria’s hospitals. In April that year, the Austin, the Royal Melbourne and Western Health had plans to double or triple their ICU capacity, and The Alfred was remodelling the entire second floor of the hospital into a dedicated ward to treat those with COVID-19.
Loading
Associate Professor Warrillow said no Victorian who needed a bed for an emergency, whether it be COVID-19 or anything else would miss out, but he was concerned about what gets displaced as other types of healthcare are delayed.
As it was last year, he said the “greatest challenge†would be how to find enough specially trained staff to oversee any new beds.
“Ultimately it’s not going to be so much about the beds or the ventilators, it’s going to be about the nursing workforce in particular, but also the medical workforce and other specialists – our physios and pharmacists – even our cleaning staff in ICU are specially trained,†he said.
“They all have skill sets that you cannot replicate immediately.â€
Opposition health spokeswoman Georgie Crozier said the government had 18 months to prepare the Victorian health system for a large surge in COVID-19 cases “yet we find ourselves in a situation where hundreds of staff are being furloughed, staff are working overtime and becoming burnt out, and there are real concerns our health system is not readyâ€.
Stay across the most crucial developments related to the pandemic with the Coronavirus Update. Sign up for the weekly newsletter.

